This blog is educate those interested in knowing why testing is so important in the diagnosis and treatment of cancer and other blood disorders.
Thursday, July 26, 2012
Study Show What Supplements One Can Use to Reduce the Risk of Pancreatic Cancer.
A study over several years was conducted to see if certain supplements could reduce the risk of pancreatic cancer. You may already be taking these cancer reducing antioxidants on a daily basis.
Wednesday, July 18, 2012
Rheumatoid Arthritis Patients Have a Higher Risk of Developing Cancer
Persons with rheumatoid arthritis have daily struggles with severe pain and movement. Another serious downfall of the disorder is that these patients are more susceptible to develop cancer.
The association between rheumatoid arthritis (RA) and cancer is not completely clear. Some studies show an increased risk of cancer in people with rheumatoid arthritis (RA) while others show a decreased risk. But the picture becomes clearer when researchers look at specific cancer types.
Lymphoma. The strongest evidence of a link appears to be between lymphoma -- the most common type of blood cancer -- and severe rheumatoid arthritis (RA). Researchers from Sweden examined data from nearly 75,000 RA patients, 378 of whom had lymphoma. The researchers assessed risk for three different levels of disease activity (low, moderate, and severe) and found that people with moderate disease activity were eight times more likely to have lymphoma than those who had low disease activity, while those with severe disease activity were 70 times more likely.
More support for a connection comes from a review of 21 published studies, including the Swedish study and 13 others that tried to determine whether there was a link between lymphoma and rheumatoid arthritis (RA). The findings, reported recently in Arthritis Research & Therapy,showed that overall, people with rheumatoid arthritis (RA) were twice as likely as the general population to develop lymphoma, particularly Hodgkin's lymphoma (one of the most curable types of cancer when detected early).
Lung cancer. The same review also reported that lung cancer was observed more often in people with rheumatoid arthritis (RA). Based on data from 12 studies, people with rheumatoid arthritis (RA) were 63% more likely to develop lung cancer than the general population.
Cancer at other sites. In addition, the authors of the review reported a potentially reduced risk of colorectal cancer among people with rheumatoid arthritis (RA) -- possibly due to their increased use of nonsteroidal antiinflammatory drugs (NSAIDs) and COX-2 inhibitors. The researchers also reported a slightly reduced risk of breast cancer.
What's Behind the Link? An important question that remains unanswered is whether people with rheumatoid arthritis (RA) are more prone to develop certain cancers than others or if the medications they take could be responsible for the increased risk.
In the Swedish study, more than 70% of people with rheumatoid arthritis (RA) had taken traditional disease-modifying antirheumatic drugs, or DMARDs, such as methotrexate (Rheumatrex, Trexall). However, the only DMARD linked to an increased risk of lymphoma was azathioprine (Imuran) -- a treatment that is rarely used today. There was also no link between NSAIDs like aspirin and ibuprofen (Advil and others).
One encouraging finding was that people who frequently used corticosteroids for inflamed joints had a lower risk of lymphoma, a result that suggests anti-inflammatory drugs could possibly protect against lymphoma.
Kimme L. Hyrich,M.D.,Arthritis Research UK Epidemiology Unit at University of Manchester discusses the risk of rheumatoid arthritis patients.
All RA patients should be regularly tested for cancer. All health care professionals should be aware of this risk and write orders so they can be screened. If you know anyone with RA please ask and encourage them to be tested. Early detection can save a life.
http://www.johnshopkinshealthalerts.com/reports/arthritis/3308-1.html
Wednesday, July 11, 2012
Chemotherapy Can Extend a Patient's Life Who Has Rare Pancreatic Cancer
When a patient has pancreatic cancer most will do what it take to extend their life. There is a rare pancreatic cancer called periampullary adenocarcinoma in which chemotherapy will increase the patient's life span.
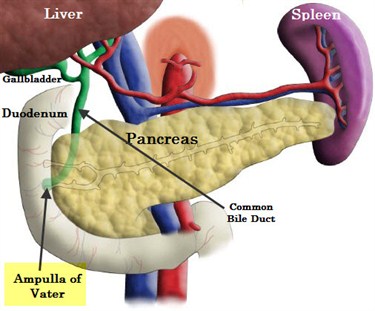
Ampullary cancer is a malignant tumor that arises from the Ampulla of Vater, the last centimeter of the common bile duct as it passes through the duodenum, the first section of the intestine. All pancreatic and biliary secretions enter the duodenum through the Ampulla of Vater.

A tumor blocking the Ampulla of Vater will interfere with drainage of the pancreatic and biliary secretions into the intestine. Jaundice results when the drainage of bile into the duodenum is blocked causing it to accumulate in in the bloodstream. Jaundice, the yellowing of the skin, is typically one of the first symptoms present with Ampullary cancer.
The diagnostic tests used to for ampullary cancer are similar to those for pancreatic cancer; endoscopy or endoscopic retrograde cholangiopancreatography (ERCP) are frequently used to make the diagnosis.
Histology of Periampullay adenocarcinoma
Patients with periampullary cancer who received chemotherapy and surgery lived longer than patients who did not receive the chemotherapy.
This is the finding of a large multi-center research effort that was published in the July 11 issue of JAMA (Journal of the American Medical Association).
This an important large international multi-center study showing the benefit of chemotherapy after surgical resection of a specific type ofperiampullary cancer," James Farrell, MD, director of the University of California Los Angeles Medical Center Endoscopic Ultrasound Division of Digestive Diseases, told dailyRx in an email,
"It supports the use of adjuvant treatment with gemcitabine for this group of patients," Dr. Farrell said.
Additional study is needed to learn more about this treatment option. "There were different survival outcomes by tumor type, although age, poorly differentiated tumor grade, and lymph node involvement were also independent survival factors,” the authors write.
Tuesday, June 26, 2012
A Rare Cancer in Children
It is always heartbreaking when children have cancer. Usually cancer in children affects the blood cells or brain. A very rare cancer in children is rhabdomyosarcoma. Where is this cancer located in a child's body?
Fewer than 60 children are diagnosed with rhabdomyosarcoma in the UK each year. About the same number in the United States. Most of them are younger than 10 years old. It's more common in boys than girls.
Rhabdomyosarcoma is the most common of the soft tissue sarcomas in children. These tumors develop from muscle or fibrous tissue and can grow in any part of the body.
The most common areas of the body to be affected are around the head and neck, the bladder or the testes. Sometimes tumours are also found in a muscle or a limb, in the chest or in the abdominal wall. If the tumour is in the head or neck region, it can occasionally spread into the brain or the fluid around the spinal cord.
What causes this disease is unknown. Children who have rare genetic disorders are more prone to have rhabdommyosarcoma.
Image of rhabdomyosarcoma that has been removed from a child's body.
The images of the children with this cancer are very disturbing so they will not be displayed.
The signs and symptoms will depend on the part of the body that's affected by the rhabdomyosarcoma. The most common sign is a swelling or lump.
Various tests may be done to check the exact size of the tumour and whether it has spread to any other part of the body. These may include:
Rhabdomyosarcomas are rare tumours and should be treated at specialist centres.
Treatment depends upon the size of the tumour, its position within the body, and whether it has spread. Treatment of rhabdomyosarcoma usually includes surgery, radiotherapy or chemotherapy, or a combination of these treatments.
Chemotherapy can make your child feel better by relieving the symptoms of the cancer, but it can sometimes have side effects such as feeling sick (nausea) and being sick (vomiting), hair loss, an increased risk of infection, bruising and bleeding, tiredness and diarrhoea.
Late side effects
A small number of children may develop side effects many years after their treatment for a rhabdomyosarcoma. Long-term side effects depend on the type of treatment used, and may include a possible reduction in bone growth, infertility,
a change in the way the heart and the kidneys work, and a slight
increase in the risk of developing another cancer in later life.
Your child’s doctor or nurse will talk to you about any possible late side effects. There is more detailed information about these late side effects in the booklet A parent’s guide to children’s cancer.
Mayo Clinic Oncologist Explains Rhabdomyosarcoma
Holly's Journey Dealing With This Rare Cancer
http://www.macmillan.org.uk/Cancerinformation/Cancertypes/Childrenscancers/Typesofchildrenscancers/Rhabdomyosarcoma.aspx
Fewer than 60 children are diagnosed with rhabdomyosarcoma in the UK each year. About the same number in the United States. Most of them are younger than 10 years old. It's more common in boys than girls.
Rhabdomyosarcoma is the most common of the soft tissue sarcomas in children. These tumors develop from muscle or fibrous tissue and can grow in any part of the body.
The most common areas of the body to be affected are around the head and neck, the bladder or the testes. Sometimes tumours are also found in a muscle or a limb, in the chest or in the abdominal wall. If the tumour is in the head or neck region, it can occasionally spread into the brain or the fluid around the spinal cord.
What causes this disease is unknown. Children who have rare genetic disorders are more prone to have rhabdommyosarcoma.
Image of rhabdomyosarcoma that has been removed from a child's body.
The images of the children with this cancer are very disturbing so they will not be displayed.
The signs and symptoms will depend on the part of the body that's affected by the rhabdomyosarcoma. The most common sign is a swelling or lump.
- If the tumor is in the head area, it can sometimes cause a blockage (obstruction) and a discharge from the nose or throat. Occasionally, an eye may appear swollen and protruding.
- If the tumor is in the abdomen (tummy), your child may have discomfort in the abdomen and difficulty going to the toilet.
- If the tumor is in the bladder, your child may have blood in the urine and difficulty passing urine.
Various tests may be done to check the exact size of the tumour and whether it has spread to any other part of the body. These may include:
- a chest x-ray to check the lungs
- an ultrasound
- CT or MRI scans
- blood and bone marrow tests.
Rhabdomyosarcomas are rare tumours and should be treated at specialist centres.
Treatment depends upon the size of the tumour, its position within the body, and whether it has spread. Treatment of rhabdomyosarcoma usually includes surgery, radiotherapy or chemotherapy, or a combination of these treatments.
Surgery
If at all possible, surgery will be used to remove the tumour. Chemotherapy, using a combination of drugs, is often given before surgery to shrink the tumour. Radiotherapy may also be given to the area of the tumour, particularly if it cannot be completely removed by surgery.Chemotherapy
If the tumour cannot be removed with surgery, treatment will usually involve a combination of chemotherapy and radiotherapy. Chemotherapy is the use of anti-cancer (cytotoxic) drugs to destroy cancer cells and is usually given every three weeks. It may be given to shrink the tumour before surgery or with radiotherapy when the tumour can't be removed by surgery. The drugs used and the length of treatment depends on the type and stage of the rhabdomyosarcoma.Radiotherapy
Radiotherapy treats cancer by using high-energy rays, which destroy the cancer cells while doing as little harm as possible to normal cells. It's given to the area where the rhabdomyosarcoma occurs.Side effects of treatment
Treatment for rhabdomyosarcoma often causes side effects, and your child’s doctor will discuss this with you before treatment starts. Any possible side effects will depend on the particular treatment being given and the part of the body that's being treated.Chemotherapy can make your child feel better by relieving the symptoms of the cancer, but it can sometimes have side effects such as feeling sick (nausea) and being sick (vomiting), hair loss, an increased risk of infection, bruising and bleeding, tiredness and diarrhoea.
Late side effects
A small number of children may develop side effects many years after their treatment for a rhabdomyosarcoma. Long-term side effects depend on the type of treatment used, and may include a possible reduction in bone growth, infertility,
a change in the way the heart and the kidneys work, and a slight
increase in the risk of developing another cancer in later life.
Your child’s doctor or nurse will talk to you about any possible late side effects. There is more detailed information about these late side effects in the booklet A parent’s guide to children’s cancer.
http://www.macmillan.org.uk/Cancerinformation/Cancertypes/Childrenscancers/Typesofchildrenscancers/Rhabdomyosarcoma.aspx
Monday, June 25, 2012
New Biomarkers Tests for Ovarian Cancer
Great new article about new biomarker testing at the end of this year concerning ovarian cancer. Every woman needs to read this to educate yourself and share with others about what is involved with this life threatening cancer.
Autotelic Lab, Fountain Valley, a developer of quantitative rapid tests, announced today that it will be presenting a poster “The Hormones BNP and FSH in Ovarian Cancer: Potential as Diagnostic Biomarkers” at ENDO 2012. Ovarian cancer accounts for approximately 3 percent of all cancers in women and is the fifth leading cause of cancer-related death among women in the United States. Ovarian cancer has the highest mortality of all cancers of the female reproductive system. This reflects, in part, a lack of early symptoms and effective ovarian cancer screening tests. Thus, ovarian cancer is often diagnosed at an advanced stage, after the cancer has spread beyond the ovary. Cancer Antigen 125 (CA125, aka Mucin16) is overproduced by ovarian cancer cells; however, it cannot be used as a diagnostic biomarker for ovarian cancer as it can be absent when disease is present, or levels can be high when no disease or no malignant disease exists. Serial changes in CA125 levels, if elevated, however, can be useful in assessment of disease status and progression. Ovarian epithelial cancer is more common in individuals with elevated Gonadotropin-releasing hormones (GnRH) including Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH) such as postmenopausal women or women who have received treatment to induce ovulation. Conversely, reduced risk of ovarian cancer is associated with a history of multiple pregnancies, breastfeeding, oral contraceptive use, and estrogen replacement therapy, all of which are related to lower levels of and reduced exposure to FSH and LH. FSH regulates gene expression in ovarian tumors and causes neovascularization of ovarian cancers by increasing Vascular Endothelial Growth Factor (VEGF) expression through upregulation of survivin. We therefore examined FSH levels in relation to CA125 as potential diagnostic marker for ovarian cancer using a quantitative point-of-care device for FSH that was recently developed for therapeutic drug monitoring. The surprising potential of FSH and/or Brain Natriuretic Peptide (BNP) as diagnostic biomarkers for ovarian cancer will be presented.
These tests are performed on serum from a blood draw. It usually take a few days to get the results,but are very informative for the oncologist as far as plan of treatment.
An Inspiring Story of a woman (physician) Diagnosed With Ovarian
Cancerhttp://news.topwirenews.com/2012/06/23/fsh-and-bnp-as-potential-diagnostic-biomarker-for-ovarian-cancer/%
Autotelic Lab, Fountain Valley, a developer of quantitative rapid tests, announced today that it will be presenting a poster “The Hormones BNP and FSH in Ovarian Cancer: Potential as Diagnostic Biomarkers” at ENDO 2012. Ovarian cancer accounts for approximately 3 percent of all cancers in women and is the fifth leading cause of cancer-related death among women in the United States. Ovarian cancer has the highest mortality of all cancers of the female reproductive system. This reflects, in part, a lack of early symptoms and effective ovarian cancer screening tests. Thus, ovarian cancer is often diagnosed at an advanced stage, after the cancer has spread beyond the ovary. Cancer Antigen 125 (CA125, aka Mucin16) is overproduced by ovarian cancer cells; however, it cannot be used as a diagnostic biomarker for ovarian cancer as it can be absent when disease is present, or levels can be high when no disease or no malignant disease exists. Serial changes in CA125 levels, if elevated, however, can be useful in assessment of disease status and progression. Ovarian epithelial cancer is more common in individuals with elevated Gonadotropin-releasing hormones (GnRH) including Follicle Stimulating Hormone (FSH) and Luteinizing Hormone (LH) such as postmenopausal women or women who have received treatment to induce ovulation. Conversely, reduced risk of ovarian cancer is associated with a history of multiple pregnancies, breastfeeding, oral contraceptive use, and estrogen replacement therapy, all of which are related to lower levels of and reduced exposure to FSH and LH. FSH regulates gene expression in ovarian tumors and causes neovascularization of ovarian cancers by increasing Vascular Endothelial Growth Factor (VEGF) expression through upregulation of survivin. We therefore examined FSH levels in relation to CA125 as potential diagnostic marker for ovarian cancer using a quantitative point-of-care device for FSH that was recently developed for therapeutic drug monitoring. The surprising potential of FSH and/or Brain Natriuretic Peptide (BNP) as diagnostic biomarkers for ovarian cancer will be presented.
These tests are performed on serum from a blood draw. It usually take a few days to get the results,but are very informative for the oncologist as far as plan of treatment.
Cancerhttp://news.topwirenews.com/2012/06/23/fsh-and-bnp-as-potential-diagnostic-biomarker-for-ovarian-cancer/%
Labels:
biomarkers,
BNP,
diagram,
FSH,
lab,
ovarian cancer,
survivor,
testing,
video
Monday, June 18, 2012
Blood Test and Early Stage Breast Cancer
Through cancer research it has been determined that a current blood test can determine which patients who were diagnosed with early stages of breast cancer and who had their tumors surgically removed may see their cancer return.
The following study will explain how this was determined.
The following study will explain how this was determined.
Doctors at the M.D. Anderson Cancer Center in Houston, Texas, took blood samples from 302 women with stage 1, 2 or 3 breast cancer right before they had their tumor surgically removed. None of the women had been treated with chemotherapy. The patients' progress was followed for nearly 3 years (35 months).
According to the study published Tuesday in the journal Lancet Oncology , 25% of women whose cancer was confined to the breast had at least one circulating tumor cell in their 7.5 milliliter sample of blood (about the equivalent of half a tablespoon). Normally a lymph node biopsy is used to determine the likelihood of the cancer coming back.
Researchers found 73 women (24%) had at least one circulating tumor cell; 29 women (about 10%) had at least two circulating tumor cells in their sample and 16 (5%) had at least 3 or more tumor cells in their blood sample.
Women with early stage breast cancer aren't usually thought to be at high risk for having their cancer come back, but some do and doctors don't know why, which is why lead study author Dr. Anthony Lucci says he and his colleagues decided to investigate this.
The study found that if a women had just one circulating tumor cell in her sample, she had a 4 times greater chance of dying, compared to a woman with no CTCs.
"If three or more tumor cells were found in a blood sample, the woman had an almost 11 times higher risk of dying from the cancer compared to those who didn't have any circulating tumor cells," says Lucci.
All in all, 31% of the women in this study found their cancer came back or died during the study period.
Lucci likens circulating tumor cells to seeds in a garden. If you dump a bag of seeds in the dirt, he says, the odds that one or several take hold and grow is much higher than planting just one seed.
Circulating Tumor Cells
"While the findings of an association between circulating tumor cells and outcome in breast cancer is not novel," says Dr. Boris Pasche, Director of the Division of Hemotology and Oncology at the University of Alabama at Birmingham. "The strength of this new paper is its capability to characterize the magnitude of the impact of CTCs on breast cancer outcome." He says the other strength of this study is that the blood samples were taken just before surgery, giving a more accurate picture of where traces of cancer are outside the breast.
Once a tumor is removed, it's possible for cells to break off, thus skewing the accuracy of how much cancer is already circulating outside the breast.
According to a commentary in the Journal of the American Medical Association in March 2010 , the first documented research on circulating tumors was conducted in 1846. Since then, studies have shown that looking for circulating tumor cells in patients, who've already seen their cancer spread, can be an important tool to determine how a patient does in the future.
This hasn't been proven to be the case for early stage breast cancer, where the cancer has not spread beyond the breast and it is something this new study doesn't do either.
However, Pasche, who was not involved with the research, says if the results are validated in larger clinical trials, this may lead to a new screening method for predicting which women may be more likely to see their cancer come back.
"This provides a new train of thought of how we should handle women with early-stage breast cancer because we could identify the women who have a high risk of recurrences and early death and treat them differently." Pasche suggests those patients get more aggressive removal of lymph nodes, they may be put on chemotherapy (something they may not normally be prescribed) and their doctors will probably have a much tighter follow-up schedule for them.
Lucci and Pasche say this type of screening is not yet ready for prime time, and M.D. Anderson already has further studies underway.
Circulating Tumor Cells and Breast Cancer Recurrencehttp://www.wtnh.com/dpps/health/cancer/blood-test-may-signal-breast-cancers-return_4198976#.T9-D67UTpJs
Wednesday, June 13, 2012
What is Happening Now In Cancer Research
Research for a cure for cancer is moving at a rapid pace. Labs are thinking outside the box and finding ways to kill cancer cells of one's type of cancer. . Areas of active basic cancer research in the Department of Molecular and Cell Biology include tumor cell biology; the use of model systems to discover novel genes involved in carcinogenesis; tumor immunology and immunotherapeutics; and structural biology of protein targets for cancer therapeutics.
Cancer arises by a multi-step involving the accumulation of activating mutations in proto-oncogenes and inactivating mutations in tumor suppressor genes. The process is accelerated by the genetic instability of cancer cells, which is believed to result from passage through “telomere crisis.” Thus, cancer cells may contain many – perhaps hundreds – of genetic changes. One of the challenges we now face is to be able to develop a complete description of the genetic changes that have taken place in each individual tumor, so that therapies can be targeted that are specific for the tumors of each individual patient.
Tumor Genetics-Sloan Kettering
Below is a chart of Tumor Immunology
Cancer arises by a multi-step involving the accumulation of activating mutations in proto-oncogenes and inactivating mutations in tumor suppressor genes. The process is accelerated by the genetic instability of cancer cells, which is believed to result from passage through “telomere crisis.” Thus, cancer cells may contain many – perhaps hundreds – of genetic changes. One of the challenges we now face is to be able to develop a complete description of the genetic changes that have taken place in each individual tumor, so that therapies can be targeted that are specific for the tumors of each individual patient.
Below is a chart of Tumor Immunology
Prof. Ofer Mandelboim, IMRIC Researcher - General and Tumour Immunology - 1 of 3
Subscribe to:
Posts (Atom)








